Digital Medicine
In the quest to provide individualized medicine, knowing the biology of a person via genomics (and all the “omics” including proteomics, metabolomics, epigenomics, and “biomarkers”) is one essential step. The other equally critical step is truly understanding the unique intricacies of a specific individual’s physiology. This has only now become possible through the development of wearable wireless sensor technology and other innovative mobile health (mHealth) technologies. Critical physiologic metrics that were once only possible to be measured in a doctor’s office or hospital setting can now be measured at home during routine activities with a level of accuracy and continuity that could previously only be found in intensive care units: metrics such as blood pressure, heart rhythm and rate, oxygen saturation in the blood, stress levels, and many more. Not only do these novel mobile technologies allow for greater convenience but they also exponentially increase our ability to more fully understand the daily individual variability in these various metrics in a manner not previously possible. This capability will allow for the greater refinement of existing phenotypes allowing for the much greater individualization of the prevention and management of multiple chronic and acute conditions.
For example, if we know someone has a genomic risk for diabetes, we can use a continuous glucose sensor to hopefully prevent the condition from ever manifesting. Or an individual with early hypertension, or with a genetic predisposition for it, can have their blood pressure monitored in a non-obtrusive, continuous manner such the daily events that influence their blood pressure can be identified and addressed through various techniques. New ways to screen breast cancer with wireless ultrasound imaging can potentially be used for women with high genomic susceptibility. By coupling genomics and wireless we are bringing two exceptionally powerful tools together to define each person at unprecedented levels with the ultimate goal of the prevention of disease and preservation of health.
Thanks to a generous grant from Qualcomm, the Digital Medicine Division of the Scripps Translational Science Institute was initiated in early 2013 under the leadership of Dr. Eric Topol, who recruited Dr. Steve Steinhubl to lead it in July 2013.
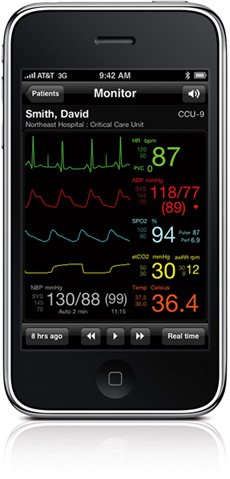 Wireless device for remote monitoring of all vital signs of hospitalized patients.
Wireless device for remote monitoring of all vital signs of hospitalized patients.
